Asking someone what they do for a living seems like an innocent question. However, people always are surprised when I explain what exactly what line of work I”m in. I get a range of responses when I meet someone new and answer that question 😊. Their responses can range from “That’s amazing! I had no idea something like that existed!” to the silent nod, confused look, maybe a polite “that’s interesting” then silence for the remainder of the 4 hour flight (yes, that really happened).
Outside of general small talk, this is one of the most common questions I receive. Not only are patients unsure what is involved with pelvic health physical therapy (also referred to as pelvic floor physical therapy, women’s health or urogynecologic therapy), but even many providers don’t fully understand the scope of what pelvic health therapy can address for a patient. The symptoms one may experience in this area can be very foreign, confusing and is definitely not well talked about…even for medical providers. For that reason, we’re going to start with the basics….
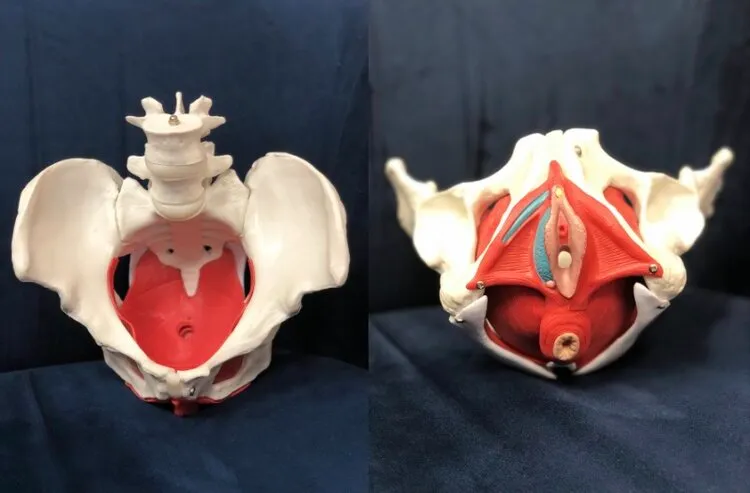
What is the pelvic floor?
The pelvic floor is a group of muscles that line the bowl of the pelvis and help with many basic functions such as bowel, bladder and sexual control. However, because of their intricate connections to other areas, there’s a strong influence into the digestive tract, general posture, the spine, the breath and more. Both men and women have a pelvic floor and yes, both men and women can struggle with symptoms from this area. The majority of what will be covered in the blogs will be discussing symptoms specific to women as this is my primary population of care, though I do treat men as well.
The muscles of the pelvic floor and adjacent muscles may be tight, weak or a combination of that. Determining exactly which muscles are tight or weak and prioritizing the order in which to address them can be pivotal to successful treatment.
What is involved with an exam for pelvic health therapy?
Some pelvic health therapists do not do an internal exam and only assess externally (looking at the perineum, or the external area between the pubic bone and the tailbone, as well as the external boney alignment). Though you can gather a lot of information with an external exam, personally I find doing an internal pelvic floor exam is a key piece of an exam to gather information from all potential areas that may be influencing a person’s symptoms. An internal pelvic floor exam performed by a pelvic health therapist is much different than that of an OBGYN, midwife or other physician doing a woman’s “annual” exam (though they’re not quite annual any longer). For one, a pelvic health therapist doesn’t use a speculum. We assess with a single, gloved finger and with our assessment, we’re not necessarily looking for a pathology of the tissue, doing a PAP smear, etc. Rather, we are looking at the muscles, tissues and boney structures to determine if there are areas of tightness, tenderness or irritation, both external and internal to the vaginal canal. The goal of the exam is to determine what the driver of the person’s symptoms is and where is it coming from so that we can address it more effectively.
During the exam, we want to see the person’s ability to contract the pelvic floor muscles (ie, Kegel) and how well they relax. Our society’s conversation around the pelvic floor, for the most part, is around Kegels and how they should be done in pregnancy and after delivery. That is a great rule of thumb, however, it is imperative that a woman be assessed by a pelvic health therapist or other medical provider to determine if it truly is appropriate for them to be doing Kegels. Sometimes, Kegels may make a person’s symptoms worse. For some people, the key thing I want them to focus on is their ability to relax the pelvic floor muscles. This can be very challenging for some people, yet imperative to successfully addressing the symptoms. If a provider is not well educated, they may suggest the patient do Kegels, when in reality that is the opposite of what they should be doing.
After looking at the health of the tissue and the person’s ability to Kegel properly, I next want to assess the person’s pelvic organ position, also known as prolapse. I will write another detailed post on pelvic organ prolapse another day. For now, the gist of this is that a person (women more than men) can have a change in the position of a pelvic organ within the pelvis itself. This can be due to pregnancy, change in hormones (pregnancy or menopause), trauma, surgery, poor bathroom habits and more). Prolapse can interfere with a person’s comfort level in day to day activities, recreational activities, intercourse as well as influence a person’s bathroom habits. Though we aren’t going to truly fix a pelvic organ prolapse, we can do a lot to help support it and minimize it from getting worse, avoid surgery and minimize the symptoms you may be experiencing.
There you have it! That is your basic pelvic exam from a pelvic health therapist. However, there is still more to it the FULL assessment of a body. Not only does a person’s posture influence their pelvic floor, but so does their abdominal organ mobility, core strength, hip strength, soft tissue mobility and breath pattern. So we have to look at and fully assess all of those areas as well. For an individual who is concerned with diastasis recti, this is imperative (more details in an another post later). For people concerned with diastasis recti, we especially want to assess the small intestine’s mobility, their breath pattern and their ability to isolate the appropriate muscles for strengthening (transverse abdominis is one of the key ones!).
If the patient is experiencing pain in the pelvis, I often get the anxious question of “Is the exam going to hurt?”. NO is the short answer. Though we may find areas of tenderness we immediately begin treating in order to help ease any discomfort and calm the system. I’m more interested in how the body responds with the adjustment of the tissues and organs than I am in the specific muscles involved.
There is a lot to look at. That is why the initial evaluation at Treasure Valley Pelvic Health is so long (approximately 90 minutes). We dive into a great deal of medical history that many other providers don’t correlate to the pelvic floor function as well as other stressors in a person’s life, behaviors and patterns that may influence their overall function. Communication with the patient, their providers and setting appropriate goals in order to help them succeed is imperative. It is our belief that in order to be the most successful, we have to meet the patient at their goals and ability to help them work through any sort of limitations in their world. Perhaps it’s stress, time management, learning how to incorporate the exercises and techniques into their day, etc. We’re only as good of therapists as we are able to help guide a patient towards success. Not just inundate them with exercises and to do’s.
The other unique part of Treasure Valley Pelvic Health is that we offer services at our clinic or also at the patient’s home (or gym!). Our goal is to provide excellent services and make the services as accessible as possible. This has been a great option for many busy Mama’s or especially for the early postpartum period when you’re a bit more hesitant to take your newborn out and about in the community. We have gone to gyms and assessed a patient during the activity they are struggling with the most or what to most improve on. It give us clear access to the person’s movements (good and bad!) in order to better guide the patient towards success.
If you have any questions about our treatments, have specific questions regarding symptoms you may be experiencing or want to learn more give us a call at 208.991.4526 or request a phone consultation using the link below.